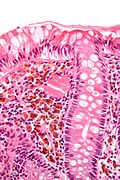
Pseudomelanosis coli
Jump to navigation
Jump to search
| Pseudomelanosis coli | |
|---|---|
| Diagnosis in short | |
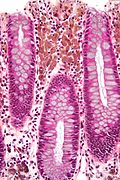
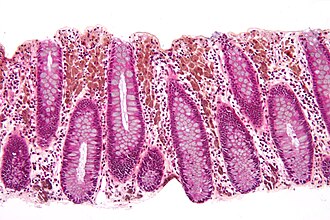 Pseudomelanosis coli. H&E stain. | |
|
| |
| LM | brown granular pigment in the lamina propria, abundant |
| LM DDx | hemorrhage, melanocytic lesion (rarely) |
| Stains | PAS +ve, Prussian blue -ve |
| Site | colon, cecum, occasionally small intestine |
|
| |
| Clinical history | use of laxatives and herbals |
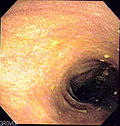
| Endoscopy | brown discolouration of the mucosa, esp. proximal colon and cecum |
| Prognosis | benign |
| Clin. DDx | colitis |
| Pseudomelanosis coli | |
|---|---|
| External resources | |
| Wikipedia | melanosis coli |
Pseudomelanosis coli, also known as melanosis coli,[1] is a relatively common benign change seen in the colon.
General
- Not melanin as the name melanosis coli suggests; it is actually lipofuscin (in macrophages).[2]
- Endoscopist may see brown pigmentation of mucosa and suspect the diagnosis.
- Presence may lead to endoscopic misinterpretation of colitis severity.[3]
Epidemiology
- Classically associated with anthracene containing laxative (e.g. Senokot) use and herbal remedies.[2]
- May be seen in individuals not using laxatives.[4]
- Seen in (long-standing) inflammatory bowel disease, especially ulcerative colitis.[4]
Gross
- Brown pigmentation of the mucosa, especially cecum and proximal colon.[2]
- Less pigmentation distal.
Note:
- May also been seen in the small intestine.[2]
Endoscopic image
Microscopic
Features:
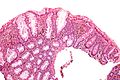
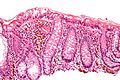
- Brown granular pigment - in the lamina propria.
- Typically more prominent in the cecum and proximal colon.[2]
Notes:
- DDx of brown pigment:
- Lipofuscin - comes with age (can be demonstrated with a PAS stain[5] or Kluver-Barrera stain[6]).
- Melanosis coli.
- Old haemorrhage, i.e. hemosiderin-laden macrophages (may be demonstrated with Prussian blue stain[7]).
- Melanin (from melanocytes) - rare in colon (may be demonstrated with a Fontana-Masson stain[8] -- though not so useful in the GI tract).
- Foreign material (e.g. tattoo pigment) - not seen in GI tract.
- Lipofuscin - comes with age (can be demonstrated with a PAS stain[5] or Kluver-Barrera stain[6]).
Images
Another case:
Stains
Sign out
ASCENDING COLON, BIOPSY: - PSEUDOMELANOSIS COLI. - NEGATIVE FOR ACTIVE COLITIS. - NEGATIVE FOR DYSPLASIA.
See also
References
- ↑ URL: http://www.medicinenet.com/melanosis_coli/article.htm. Accessed on: 4 March 2011.
- ↑ 2.0 2.1 2.2 2.3 2.4 Freeman HJ (July 2008). ""Melanosis" in the small and large intestine". World J. Gastroenterol. 14 (27): 4296-9. PMID 18666316. http://www.wjgnet.com/1007-9327/14/4296.asp. Cite error: Invalid
<ref>tag; name "pmid18666316" defined multiple times with different content - ↑ Zapatier, JA.; Schneider, A.; Parra, JL. (Dec 2010). "Overestimation of ulcerative colitis due to melanosis coli.". Acta Gastroenterol Latinoam 40 (4): 351-3. PMID 21375218.
- ↑ 4.0 4.1 Pardi, DS.; Tremaine, WJ.; Rothenberg, HJ.; Batts, KP. (Apr 1998). "Melanosis coli in inflammatory bowel disease.". J Clin Gastroenterol 26 (3): 167-70. PMID 9600362.
- ↑ Kovi J, Leifer C (July 1970). "Lipofuscin pigment accumulation in spontaneous mammary carcinoma of A/Jax mouse". J Natl Med Assoc 62 (4): 287–90. PMC 2611776. PMID 5463681. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2611776/pdf/jnma00512-0077.pdf.
- ↑ URL: http://education.vetmed.vt.edu/curriculum/VM8054/labs/Lab2/Examples/exkluvbarr.htm. Accessed on: 5 May 2010.
- ↑ URL: http://education.vetmed.vt.edu/curriculum/VM8054/labs/Lab2/Examples/exprussb.htm. Accessed on: 5 May 2010.
- ↑ URL: http://education.vetmed.vt.edu/curriculum/VM8054/labs/Lab2/Examples/exfontana.htm. Accessed on: 5 May 2010.
- ↑ Benavides SH, Morgante PE, Monserrat AJ, Zárate J, Porta EA (August 1997). "The pigment of melanosis coli: a lectin histochemical study". Gastrointest. Endosc. 46 (2): 131–8. PMID 9283862.