Difference between revisions of "Eosinophilic esophagitis"
Jump to navigation
Jump to search
(+cat.) |
(split-out) |
||
| Line 1: | Line 1: | ||
# | '''Eosinophilic esophagitis''', abbreviated '''EE''', is relatively uncommon pathology of the [[esophagus]] with some similarities to [[gastroesophageal reflux disease]] (GERD). | ||
==General== | |||
*The current thinking is that it is a clinico-pathologic diagnosis.<ref name=pmid20524860>{{Cite journal | last1 = Genevay | first1 = M. | last2 = Rubbia-Brandt | first2 = L. | last3 = Rougemont | first3 = AL. | title = Do eosinophil numbers differentiate eosinophilic esophagitis from gastroesophageal reflux disease? | journal = Arch Pathol Lab Med | volume = 134 | issue = 6 | pages = 815-25 | month = Jun | year = 2010 | doi = 10.1043/1543-2165-134.6.815 | PMID = 20524860 | url = http://www.archivesofpathology.org/doi/full/10.1043/1543-2165-134.6.815 }}</ref> | |||
Clinical: | |||
*Dysphagia<ref>URL: [http://www.medicinenet.com/eosinophilic_esophagitis/page2.htm#tocc http://www.medicinenet.com/eosinophilic_esophagitis/page2.htm#tocc]. Accessed on: 1 December 2009.</ref> - classic presentation. | |||
*Dyspepsia. | |||
**Often mimics [[gastroesophageal reflux disease]] (GERD).<ref name=pmid19596009>{{Cite journal | last1 = Rothenberg | first1 = ME. | title = Biology and treatment of eosinophilic esophagitis. | journal = Gastroenterology | volume = 137 | issue = 4 | pages = 1238-49 | month = Oct | year = 2009 | doi = 10.1053/j.gastro.2009.07.007 | PMID = 19596009 }}</ref> | |||
Treatment: | |||
*Avoid exacerbating antigens. | |||
*Topical corticosteroids, e.g. fluticasone. | |||
*Do not respond to proton pump inhibitors. | |||
Biopsies: | |||
*Should be taken from: upper, mid, lower and submitted in separate containers (eosinophilia present through-out-- to differentiate from GERD). | |||
Associations: | |||
*Atopy.<ref name=Ref_GLP19>{{Ref GLP|19}}</ref> | |||
*[[Celiac disease]].<ref name=pmid19841598>{{cite journal |author=Leslie C, Mews C, Charles A, Ravikumara M |title=Celiac disease and eosinophilic esophagitis: a true association |journal=J. Pediatr. Gastroenterol. Nutr. |volume=50 |issue=4 |pages=397–9 |year=2010 |month=April |pmid=19841598 |doi=10.1097/MPG.0b013e3181a70af4 |url=}}</ref> | |||
*Oral antigens, i.e. particular foods.<ref name=pmid19596009/> | |||
*Familial association.<ref name=pmid19596009/> | |||
*Young ~ 35 years old.<ref name=pmid23382628/> | |||
*Male > female (3:1).<ref name=pmid23382628>{{Cite journal | last1 = Dellon | first1 = ES. | last2 = Erichsen | first2 = R. | last3 = Pedersen | first3 = L. | last4 = Shaheen | first4 = NJ. | last5 = Baron | first5 = JA. | last6 = Sørensen | first6 = HT. | last7 = Vyberg | first7 = M. | title = Development and validation of a registry-based definition of eosinophilic esophagitis in Denmark. | journal = World J Gastroenterol | volume = 19 | issue = 4 | pages = 503-10 | month = Jan | year = 2013 | doi = 10.3748/wjg.v19.i4.503 | PMID = 23382628 }}</ref> | |||
==Gross/endoscopic== | |||
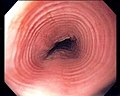
*'''Trachealization'''; eosphagus looks like trachea.<ref name=pmid19636182>{{Cite journal | last1 = Al-Hussaini | first1 = AA. | last2 = Semaan | first2 = T. | last3 = El Hag | first3 = IA. | title = Esophageal trachealization: a feature of eosinophilic esophagitis. | journal = Saudi J Gastroenterol | volume = 15 | issue = 3 | pages = 193-5 | month = | year = | doi = 10.4103/1319-3767.54747 | PMID = 19636182 }} | |||
</ref> | |||
**[[AKA]] ''feline esophagus''.<ref>URL: [http://www.ajronline.org/cgi/reprint/164/4/900.pdf http://www.ajronline.org/cgi/reprint/164/4/900.pdf]. Accessed on: 4 October 2010.</ref> | |||
*White. | |||
DDx (endoscopic): | |||
*[[Candida esophagitis]] | |||
===Image=== | |||
<gallery> | |||
Image:Multi_ring_esophagus.jpg | Trachealization of the esophagus. (WC) | |||
</gallery> | |||
*[http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2841420/figure/F0001/ Trachealization - radiograph (nih.gov)]. | |||
==Microscopic== | |||
Features:<ref name=Ref_GLP19>{{Ref GLP|19}}</ref> | |||
*Mucosa with "abundant eosinophils". | |||
*[[Basal cell hyperplasia]]. | |||
**Three cells thick ''or'' >15% of epithelial thickness. | |||
*Papillae elongated. | |||
**Papillae that reach into the top 1/3 of the epithelial layer - definition for GERD.<ref name=Ref_PBoD804>{{Ref PBoD|804}}</ref> | |||
Notes "abundant eosinophils": | |||
*Criteria for number of eosinophils/area is '''''highly variable'''''; there is a 23X fold variation in published values and only 11% of studies actually define an area (most studies, embarassing for pathologists that understand this issue, only give the number of eosinophils per "HPF")!<ref name=pmid17617209>{{cite journal |author=Dellon ES, Aderoju A, Woosley JT, Sandler RS, Shaheen NJ |title=Variability in diagnostic criteria for eosinophilic esophagitis: a systematic review |journal=Am. J. Gastroenterol. |volume=102 |issue=10 |pages=2300–13 |year=2007 |month=October |pmid=17617209 |doi=10.1111/j.1572-0241.2007.01396.x |url=}}</ref> | |||
**Interrater variability is low, i.e. good, if the procedure is standardized.<ref name=pmid19830560>{{Cite journal | last1 = Dellon | first1 = ES. | last2 = Fritchie | first2 = KJ. | last3 = Rubinas | first3 = TC. | last4 = Woosley | first4 = JT. | last5 = Shaheen | first5 = NJ. | title = Inter- and intraobserver reliability and validation of a new method for determination of eosinophil counts in patients with esophageal eosinophilia. | journal = Dig Dis Sci | volume = 55 | issue = 7 | pages = 1940-9 | month = Jul | year = 2010 | doi = 10.1007/s10620-009-1005-z | PMID = 19830560 }}</ref> | |||
*The most commonly reported cut points are 15, 20 and 24 eosinophils/HPF, without defining HPF.<ref name=pmid17617209/> | |||
**The ''Foundation Series'' book<ref name=Ref_GLP19>{{Ref GLP|19}}</ref> says: "> 20/HPF"; ''[[onlinepathology]]'' sees this definition as garbage, as "HPF" is not defined (see [[HPFitis]]). | |||
**There is a consensus paper<ref name=pmid17919504>{{cite journal |author=Furuta GT, Liacouras CA, Collins MH, ''et al.'' |title=Eosinophilic esophagitis in children and adults: a systematic review and consensus recommendations for diagnosis and treatment |journal=Gastroenterology |volume=133 |issue=4 |pages=1342–63 |year=2007 |month=October |pmid=17919504 |doi=10.1053/j.gastro.2007.08.017 |url=}}</ref> that makes note of [[HPFitis]]... and then goes on to ignore to whole issue by defining EE as 15/HPF. It blows my mind that the people could be so will fully blind and that the idiotic reviewers didn't understand this. | |||
**Most resident microscopes at the Toronto teaching hospitals have 22 mm eye pieces and have for their highest magnification objective a 40X. De facto, this means most people in Toronto are using the Liacouras ''et al.'' definition.<ref name=pmid16361045>{{cite journal |author=Liacouras CA, Spergel JM, Ruchelli E, ''et al.'' |title=Eosinophilic esophagitis: a 10-year experience in 381 children |journal=Clin. Gastroenterol. Hepatol. |volume=3 |issue=12 |pages=1198–206 |year=2005 |month=December |pmid=16361045 |doi= |url=}}</ref> | |||
*Eosinophils may be patchy.<ref name=pmid22502795>{{Cite journal | last1 = Saffari | first1 = H. | last2 = Peterson | first2 = KA. | last3 = Fang | first3 = JC. | last4 = Teman | first4 = C. | last5 = Gleich | first5 = GJ. | last6 = Pease | first6 = LF. | title = Patchy eosinophil distributions in an esophagectomy specimen from a patient with eosinophilic esophagitis: Implications for endoscopic biopsy. | journal = J Allergy Clin Immunol | volume = 130 | issue = 3 | pages = 798-800 | month = Sep | year = 2012 | doi = 10.1016/j.jaci.2012.03.009 | PMID = 22502795 }}</ref> | |||
DDx:<ref name=Ref_Odze244>{{Ref Odze|244}}</ref> | |||
*[[Gastroesophageal reflux disease]] - no mid and proximal involvement. | |||
*[[Infectious esophagitis]]. | |||
*Eosinophilic gastroenteritis. | |||
*Hypereosinophilic syndrome. | |||
===Images=== | |||
<gallery> | |||
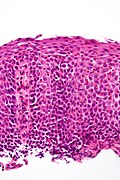
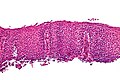
Image:Eosinophilic_esophagitis_-_2_-_very_high_mag.jpg | Eosinophilic esophagitis - very high mag. (WC) | |||
Image:Eosinophilic_esophagitis_-_2_-_high_mag.jpg | Eosinophilic esophagitis - high mag. (WC) | |||
</gallery> | |||
*[http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2841420/figure/F0003/ Eosinophilic esophagitis (nih.gov)]. | |||
*[http://www.archivesofpathology.org/action/showFullPopup?id=i1543-2165-134-6-815-f03&doi=10.1043%2F1543-2165-134.6.815 EE versus GERD (archivesofpathology.org)].<ref name=pmid20524860/> | |||
==Sign out== | |||
<pre> | |||
ESOPHAGUS, DISTAL, BIOPSY: | |||
- SQUAMOUS MUCOSA WITH BASAL CELL HYPERPLASIA, ABUNDANT INTRAEPITHELIAL EOSINOPHILS, | |||
EDEMA, AND PAPILLARY ELONGATION, SEE COMMENT. | |||
- STAINS (PAS-D, GMS) NEGATIVE FOR MICROORGANISMS. | |||
- NEGATIVE FOR INTESTINAL METAPLASIA. | |||
- NEGATIVE FOR DYSPLASIA. | |||
COMMENT: | |||
There are approximately 65 eosinophils per 0.2376 mm*mm (1 HPF). | |||
Literature valves show a large variation when defining eosinophilic esophagitis | |||
and frequently use "HPF" as a measure of area, which is not a standardized measure. | |||
[Am. J. Gastroenterol. 102 (10): 2300–13.] | |||
Common cut-points are 15 eosinophils/HPF and 20 eosinophils/HPF, where HPF is | |||
often undefined. | |||
The above findings are suggestive of eosinophilic esophagitis in the proper | |||
clinical context. | |||
</pre> | |||
===Patchy eosinophils=== | |||
<pre> | |||
ESOPHAGUS (DISTAL), BIOPSY: | |||
- SQUAMOUS MUCOSA WITH BASAL CELL HYPERPLASIA, INTRAEPITHELIAL EDEMA AND ONLY | |||
FOCALLY ABUNDANT INTRAEPITHELIAL EOSINOPHILS, SEE COMMENT. | |||
- COLUMNAR EPITHELIUM WITH MODERATE CHRONIC INFLAMMATION, AND PANCREATIC | |||
ACINAR METAPLASIA. | |||
- NEGATIVE FOR INTESTINAL METAPLASIA. | |||
- NEGATIVE FOR DYSPLASIA AND NEGATIVE FOR MALIGNANCY. | |||
COMMENT: | |||
One high power field (field diameter 0.55 mm) has 25 eosinophils. The findings are | |||
compatible with gastroesophageal reflux; however, eosinophilic esophagitis is also a | |||
consideration. Clinical correlation is required. | |||
Literature valves show a large variation when defining eosinophilic esophagitis | |||
and frequently use "HPF" as a measure of area, which is not a standardized measure. | |||
[Am. J. Gastroenterol. 102 (10): 2300 13.] | |||
Common cut-points are 15 eosinophils/HPF and 20 eosinophils/HPF, where HPF is | |||
often undefined. | |||
</pre> | |||
===Histology suggestive=== | |||
<pre> | |||
ESOPHAGUS, BIOPSY: | |||
- SQUAMOUS MUCOSA WITH MARKED BASAL CELL HYPERPLASIA, FOCALLY ABUNDANT | |||
INTRAEPITHELIAL EOSINOPHILS, EDEMA, AND PAPILLARY ELONGATION, SEE COMMENT. | |||
- NEGATIVE FOR INTESTINAL METAPLASIA. | |||
- NEGATIVE FOR DYSPLASIA. | |||
COMMENT: | |||
Focally, there are approximately 35 eosinophils per 0.2376 mm*mm (1 HPF). | |||
The above findings raise the possibility of eosinophilic esophagitis; clinical | |||
correlation is suggested. A re-biopsy including a portion of the proximal esophagus | |||
could be considered. | |||
</pre> | |||
==See also== | |||
*[[Esophagus]]. | |||
*[[Eosinophilic colitis]]. | |||
*[[Eosinophil]]. | |||
==References== | |||
{{Reflist|2}} | |||
[[Category:Diagnosis]] | [[Category:Diagnosis]] | ||
[[Category:Esophagus]] | |||
Revision as of 02:57, 10 December 2013
Eosinophilic esophagitis, abbreviated EE, is relatively uncommon pathology of the esophagus with some similarities to gastroesophageal reflux disease (GERD).
General
- The current thinking is that it is a clinico-pathologic diagnosis.[1]
Clinical:
- Dysphagia[2] - classic presentation.
- Dyspepsia.
- Often mimics gastroesophageal reflux disease (GERD).[3]
Treatment:
- Avoid exacerbating antigens.
- Topical corticosteroids, e.g. fluticasone.
- Do not respond to proton pump inhibitors.
Biopsies:
- Should be taken from: upper, mid, lower and submitted in separate containers (eosinophilia present through-out-- to differentiate from GERD).
Associations:
- Atopy.[4]
- Celiac disease.[5]
- Oral antigens, i.e. particular foods.[3]
- Familial association.[3]
- Young ~ 35 years old.[6]
- Male > female (3:1).[6]
Gross/endoscopic
DDx (endoscopic):
Image
Microscopic
Features:[4]
- Mucosa with "abundant eosinophils".
- Basal cell hyperplasia.
- Three cells thick or >15% of epithelial thickness.
- Papillae elongated.
- Papillae that reach into the top 1/3 of the epithelial layer - definition for GERD.[9]
Notes "abundant eosinophils":
- Criteria for number of eosinophils/area is highly variable; there is a 23X fold variation in published values and only 11% of studies actually define an area (most studies, embarassing for pathologists that understand this issue, only give the number of eosinophils per "HPF")![10]
- Interrater variability is low, i.e. good, if the procedure is standardized.[11]
- The most commonly reported cut points are 15, 20 and 24 eosinophils/HPF, without defining HPF.[10]
- The Foundation Series book[4] says: "> 20/HPF"; onlinepathology sees this definition as garbage, as "HPF" is not defined (see HPFitis).
- There is a consensus paper[12] that makes note of HPFitis... and then goes on to ignore to whole issue by defining EE as 15/HPF. It blows my mind that the people could be so will fully blind and that the idiotic reviewers didn't understand this.
- Most resident microscopes at the Toronto teaching hospitals have 22 mm eye pieces and have for their highest magnification objective a 40X. De facto, this means most people in Toronto are using the Liacouras et al. definition.[13]
- Eosinophils may be patchy.[14]
DDx:[15]
- Gastroesophageal reflux disease - no mid and proximal involvement.
- Infectious esophagitis.
- Eosinophilic gastroenteritis.
- Hypereosinophilic syndrome.
Images
Sign out
ESOPHAGUS, DISTAL, BIOPSY: - SQUAMOUS MUCOSA WITH BASAL CELL HYPERPLASIA, ABUNDANT INTRAEPITHELIAL EOSINOPHILS, EDEMA, AND PAPILLARY ELONGATION, SEE COMMENT. - STAINS (PAS-D, GMS) NEGATIVE FOR MICROORGANISMS. - NEGATIVE FOR INTESTINAL METAPLASIA. - NEGATIVE FOR DYSPLASIA. COMMENT: There are approximately 65 eosinophils per 0.2376 mm*mm (1 HPF). Literature valves show a large variation when defining eosinophilic esophagitis and frequently use "HPF" as a measure of area, which is not a standardized measure. [Am. J. Gastroenterol. 102 (10): 2300–13.] Common cut-points are 15 eosinophils/HPF and 20 eosinophils/HPF, where HPF is often undefined. The above findings are suggestive of eosinophilic esophagitis in the proper clinical context.
Patchy eosinophils
ESOPHAGUS (DISTAL), BIOPSY: - SQUAMOUS MUCOSA WITH BASAL CELL HYPERPLASIA, INTRAEPITHELIAL EDEMA AND ONLY FOCALLY ABUNDANT INTRAEPITHELIAL EOSINOPHILS, SEE COMMENT. - COLUMNAR EPITHELIUM WITH MODERATE CHRONIC INFLAMMATION, AND PANCREATIC ACINAR METAPLASIA. - NEGATIVE FOR INTESTINAL METAPLASIA. - NEGATIVE FOR DYSPLASIA AND NEGATIVE FOR MALIGNANCY. COMMENT: One high power field (field diameter 0.55 mm) has 25 eosinophils. The findings are compatible with gastroesophageal reflux; however, eosinophilic esophagitis is also a consideration. Clinical correlation is required. Literature valves show a large variation when defining eosinophilic esophagitis and frequently use "HPF" as a measure of area, which is not a standardized measure. [Am. J. Gastroenterol. 102 (10): 2300 13.] Common cut-points are 15 eosinophils/HPF and 20 eosinophils/HPF, where HPF is often undefined.
Histology suggestive
ESOPHAGUS, BIOPSY: - SQUAMOUS MUCOSA WITH MARKED BASAL CELL HYPERPLASIA, FOCALLY ABUNDANT INTRAEPITHELIAL EOSINOPHILS, EDEMA, AND PAPILLARY ELONGATION, SEE COMMENT. - NEGATIVE FOR INTESTINAL METAPLASIA. - NEGATIVE FOR DYSPLASIA. COMMENT: Focally, there are approximately 35 eosinophils per 0.2376 mm*mm (1 HPF). The above findings raise the possibility of eosinophilic esophagitis; clinical correlation is suggested. A re-biopsy including a portion of the proximal esophagus could be considered.
See also
References
- ↑ 1.0 1.1 Genevay, M.; Rubbia-Brandt, L.; Rougemont, AL. (Jun 2010). "Do eosinophil numbers differentiate eosinophilic esophagitis from gastroesophageal reflux disease?". Arch Pathol Lab Med 134 (6): 815-25. doi:10.1043/1543-2165-134.6.815. PMID 20524860. http://www.archivesofpathology.org/doi/full/10.1043/1543-2165-134.6.815.
- ↑ URL: http://www.medicinenet.com/eosinophilic_esophagitis/page2.htm#tocc. Accessed on: 1 December 2009.
- ↑ 3.0 3.1 3.2 Rothenberg, ME. (Oct 2009). "Biology and treatment of eosinophilic esophagitis.". Gastroenterology 137 (4): 1238-49. doi:10.1053/j.gastro.2009.07.007. PMID 19596009.
- ↑ 4.0 4.1 4.2 Iacobuzio-Donahue, Christine A.; Montgomery, Elizabeth A. (2005). Gastrointestinal and Liver Pathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Churchill Livingstone. pp. 19. ISBN 978-0443066573.
- ↑ Leslie C, Mews C, Charles A, Ravikumara M (April 2010). "Celiac disease and eosinophilic esophagitis: a true association". J. Pediatr. Gastroenterol. Nutr. 50 (4): 397–9. doi:10.1097/MPG.0b013e3181a70af4. PMID 19841598.
- ↑ 6.0 6.1 Dellon, ES.; Erichsen, R.; Pedersen, L.; Shaheen, NJ.; Baron, JA.; Sørensen, HT.; Vyberg, M. (Jan 2013). "Development and validation of a registry-based definition of eosinophilic esophagitis in Denmark.". World J Gastroenterol 19 (4): 503-10. doi:10.3748/wjg.v19.i4.503. PMID 23382628.
- ↑ Al-Hussaini, AA.; Semaan, T.; El Hag, IA.. "Esophageal trachealization: a feature of eosinophilic esophagitis.". Saudi J Gastroenterol 15 (3): 193-5. doi:10.4103/1319-3767.54747. PMID 19636182.
- ↑ URL: http://www.ajronline.org/cgi/reprint/164/4/900.pdf. Accessed on: 4 October 2010.
- ↑ Cotran, Ramzi S.; Kumar, Vinay; Fausto, Nelson; Nelso Fausto; Robbins, Stanley L.; Abbas, Abul K. (2005). Robbins and Cotran pathologic basis of disease (7th ed.). St. Louis, Mo: Elsevier Saunders. pp. 804. ISBN 0-7216-0187-1.
- ↑ 10.0 10.1 Dellon ES, Aderoju A, Woosley JT, Sandler RS, Shaheen NJ (October 2007). "Variability in diagnostic criteria for eosinophilic esophagitis: a systematic review". Am. J. Gastroenterol. 102 (10): 2300–13. doi:10.1111/j.1572-0241.2007.01396.x. PMID 17617209.
- ↑ Dellon, ES.; Fritchie, KJ.; Rubinas, TC.; Woosley, JT.; Shaheen, NJ. (Jul 2010). "Inter- and intraobserver reliability and validation of a new method for determination of eosinophil counts in patients with esophageal eosinophilia.". Dig Dis Sci 55 (7): 1940-9. doi:10.1007/s10620-009-1005-z. PMID 19830560.
- ↑ Furuta GT, Liacouras CA, Collins MH, et al. (October 2007). "Eosinophilic esophagitis in children and adults: a systematic review and consensus recommendations for diagnosis and treatment". Gastroenterology 133 (4): 1342–63. doi:10.1053/j.gastro.2007.08.017. PMID 17919504.
- ↑ Liacouras CA, Spergel JM, Ruchelli E, et al. (December 2005). "Eosinophilic esophagitis: a 10-year experience in 381 children". Clin. Gastroenterol. Hepatol. 3 (12): 1198–206. PMID 16361045.
- ↑ Saffari, H.; Peterson, KA.; Fang, JC.; Teman, C.; Gleich, GJ.; Pease, LF. (Sep 2012). "Patchy eosinophil distributions in an esophagectomy specimen from a patient with eosinophilic esophagitis: Implications for endoscopic biopsy.". J Allergy Clin Immunol 130 (3): 798-800. doi:10.1016/j.jaci.2012.03.009. PMID 22502795.
- ↑ Odze, Robert D.; Goldblum, John R. (2009). Surgical pathology of the GI tract, liver, biliary tract and pancreas (2nd ed.). Saunders. pp. 244. ISBN 978-1416040590.