Difference between revisions of "Bladder cancer staging"
Jump to navigation
Jump to search
(create) |
|||
| (7 intermediate revisions by the same user not shown) | |||
| Line 1: | Line 1: | ||
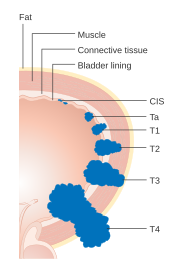
The article deals with '''bladder cancer staging'''. A general discussion | [[Image:Diagram showing the T stages of bladder cancer CRUK 372.svg|thumb|right|180px|Schematic showing the T stages in bladder cancer. (WC/CRUK)]] | ||
The article deals with '''bladder cancer staging'''. A general discussion about staging is found in ''[[cancer staging]]''. | |||
==General== | ==General== | ||
*TNM staging the most commonly used. | *TNM staging the most commonly used. | ||
*[[Urachal carcinoma]] has its own staging system - see ''[[Sheldon staging system]]''. | *[[Urachal carcinoma]] has its own staging system - see ''[[Sheldon staging system]]''.<ref name=pmid22901574>{{Cite journal | last1 = Bruins | first1 = HM. | last2 = Visser | first2 = O. | last3 = Ploeg | first3 = M. | last4 = Hulsbergen-van de Kaa | first4 = CA. | last5 = Kiemeney | first5 = LA. | last6 = Witjes | first6 = JA. | title = The clinical epidemiology of urachal carcinoma: results of a large, population based study. | journal = J Urol | volume = 188 | issue = 4 | pages = 1102-7 | month = Oct | year = 2012 | doi = 10.1016/j.juro.2012.06.020 | PMID = 22901574 }}</ref> | ||
==TNM staging system== | ==TNM staging system== | ||
| Line 10: | Line 11: | ||
! T stage | ! T stage | ||
! Criteria | ! Criteria | ||
|- | |- | ||
| | | Ta | ||
| | | non-invasive papillary carcinoma | ||
| | |- | ||
| Tis | |||
| [[urothelial carcinoma in situ|carcinoma in situ]] | |||
|- | |- | ||
| T1 | | T1 | ||
| lamina propria invasion | | lamina propria invasion | ||
|- | |- | ||
| T2 | | T2 | ||
| muscularis propria invasion | | muscularis propria invasion | ||
|- | |- | ||
| T3a | | T3a | ||
| microscopic extravesicular invasion | | microscopic extravesicular invasion | ||
|- | |- | ||
| T3b | | T3b | ||
| macroscopic extravesicular invasion | | macroscopic extravesicular invasion | ||
|- | |- | ||
| T4a | | T4a | ||
| extension into the uterus, vagina or prostate | | extension into the uterus, vagina or prostate | ||
|- | |- | ||
| T4b | | T4b | ||
| extension into the abdominal wall or pelvic wall | | extension into the abdominal wall or pelvic wall | ||
|} | |} | ||
==== | Notes: | ||
*The most important distinction is between T1 and T2. This is dealt with in the ''[[muscularis propria invasion in the urinary bladder]]'' article. | |||
**T2 is typically managed with a [[radical cystectomy]] or [[radical cystoprostatectomy]]. | |||
*Upstaging based on cystectomy/cytoprostatectomy pathology common - range 20-80%.<ref name=pmid22321341>{{Cite journal | last1 = Turker | first1 = P. | last2 = Bostrom | first2 = PJ. | last3 = Wroclawski | first3 = ML. | last4 = van Rhijn | first4 = B. | last5 = Kortekangas | first5 = H. | last6 = Kuk | first6 = C. | last7 = Mirtti | first7 = T. | last8 = Fleshner | first8 = NE. | last9 = Jewett | first9 = MA. | title = Upstaging of urothelial cancer at the time of radical cystectomy: factors associated with upstaging and its effect on outcome. | journal = BJU Int | volume = 110 | issue = 6 | pages = 804-11 | month = Sep | year = 2012 | doi = 10.1111/j.1464-410X.2012.10939.x | PMID = 22321341 }}</ref> | |||
===Nodes=== | |||
{| class="wikitable sortable" | |||
! N stage | |||
! Criteria | |||
|- | |||
| N1 | |||
| one regional [[lymph node metastasis]] | |||
|- | |||
| N2 | |||
| more than one regional lymph node metastasis | |||
|- | |||
| N3 | |||
| metastasis to the common iliac lymph nodes | |||
|} | |||
==See also== | ==See also== | ||
Latest revision as of 03:58, 9 February 2016
The article deals with bladder cancer staging. A general discussion about staging is found in cancer staging.
General
- TNM staging the most commonly used.
- Urachal carcinoma has its own staging system - see Sheldon staging system.[1]
TNM staging system
Tumour
| T stage | Criteria |
|---|---|
| Ta | non-invasive papillary carcinoma |
| Tis | carcinoma in situ |
| T1 | lamina propria invasion |
| T2 | muscularis propria invasion |
| T3a | microscopic extravesicular invasion |
| T3b | macroscopic extravesicular invasion |
| T4a | extension into the uterus, vagina or prostate |
| T4b | extension into the abdominal wall or pelvic wall |
Notes:
- The most important distinction is between T1 and T2. This is dealt with in the muscularis propria invasion in the urinary bladder article.
- T2 is typically managed with a radical cystectomy or radical cystoprostatectomy.
- Upstaging based on cystectomy/cytoprostatectomy pathology common - range 20-80%.[2]
Nodes
| N stage | Criteria |
|---|---|
| N1 | one regional lymph node metastasis |
| N2 | more than one regional lymph node metastasis |
| N3 | metastasis to the common iliac lymph nodes |
See also
References
- ↑ Bruins, HM.; Visser, O.; Ploeg, M.; Hulsbergen-van de Kaa, CA.; Kiemeney, LA.; Witjes, JA. (Oct 2012). "The clinical epidemiology of urachal carcinoma: results of a large, population based study.". J Urol 188 (4): 1102-7. doi:10.1016/j.juro.2012.06.020. PMID 22901574.
- ↑ Turker, P.; Bostrom, PJ.; Wroclawski, ML.; van Rhijn, B.; Kortekangas, H.; Kuk, C.; Mirtti, T.; Fleshner, NE. et al. (Sep 2012). "Upstaging of urothelial cancer at the time of radical cystectomy: factors associated with upstaging and its effect on outcome.". BJU Int 110 (6): 804-11. doi:10.1111/j.1464-410X.2012.10939.x. PMID 22321341.