Difference between revisions of "Parathyroid glands"
Jump to navigation
Jump to search
| (72 intermediate revisions by the same user not shown) | |||
| Line 1: | Line 1: | ||
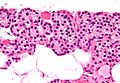
[[Image:Parathyroid gland high mag.jpg|thumb|right|280px|[[Micrograph]] of a parathyroid gland. [[H&E stain]].]] | |||
The '''parathyroid glands''' are an endocrine organ that is important in calcium regulation. They often make an appearance in the context of [[thyroid surgery]]. | The '''parathyroid glands''' are an endocrine organ that is important in calcium regulation. They often make an appearance in the context of [[thyroid surgery]]. | ||
They produce parathyroid hormone (PTH). PTH acts to increase serum calcium and is important in the regulation of the calcium balance. | |||
=Clinical= | =Clinical= | ||
== | ==Hyperparathyroidism== | ||
*Definition: increased secretion of ''parathyroid hormone'' (PTH).<ref name=emed_hyperparathyroid>URL: [http://emedicine.medscape.com/article/127351-overview http://emedicine.medscape.com/article/127351-overview]. Accessed on: 24 January 2013.</ref> | |||
What PTH does:<ref name=emed_hyperparathyroid>URL: [http://emedicine.medscape.com/article/127351-overview http://emedicine.medscape.com/article/127351-overview]. Accessed on: 24 January 2013.</ref> | |||
*Increase serum calcium. | |||
*Decrease serum phosphate. | |||
===Classification=== | ===Classification=== | ||
*Primary. | *Primary. | ||
*Secondary. | *Secondary. | ||
*Tertiary. | *Tertiary. | ||
====Overview in a table==== | |||
{| class="wikitable sortable" | |||
! Type | |||
! PTH | |||
! Calcium | |||
! Common causes | |||
|- | |||
| Primary hyperparathyroidism | |||
| high | |||
| high | |||
| [[parathyroid adenoma]] (~85-90% of cases), [[parathyroid hyperplasia]] (~10-15% of cases) | |||
|- | |||
| Secondary hyperparathyroidism | |||
| high | |||
| low or normal | |||
| chronic renal failure, vitamin D deficiency<ref name=emed_hyperparathyroid_2ndary>URL: [http://emedicine.medscape.com/article/127351-overview#aw2aab6b5 http://emedicine.medscape.com/article/127351-overview#aw2aab6b5]. Accessed on: 24 January 2013.</ref> | |||
|- | |||
| Tertiary hyperparathyroidism | |||
| high | |||
| high | |||
| persistent hyperparathyroidism after renal transplant;<ref name=emed_hyperparathyroid_tertiary>URL: [http://emedicine.medscape.com/article/127351-overview#aw2aab6b6 http://emedicine.medscape.com/article/127351-overview#aw2aab6b6]. Accessed on: 24 January 2013.</ref> arises in the context of secondary hyperparathyroidism<ref name=pmid26163537>{{Cite journal | last1 = Duan | first1 = K. | last2 = Gomez Hernandez | first2 = K. | last3 = Mete | first3 = O. | title = Clinicopathological correlates of hyperparathyroidism. | journal = J Clin Pathol | volume = 68 | issue = 10 | pages = 771-87 | month = Oct | year = 2015 | doi = 10.1136/jclinpath-2015-203186 | PMID = 26163537 }}</ref> | |||
|} | |||
====Genetics==== | |||
Genes implicated in hyperparathyroidism:<ref name=pmid22187299>{{Cite journal | last1 = Starker | first1 = LF. | last2 = Akerström | first2 = T. | last3 = Long | first3 = WD. | last4 = Delgado-Verdugo | first4 = A. | last5 = Donovan | first5 = P. | last6 = Udelsman | first6 = R. | last7 = Lifton | first7 = RP. | last8 = Carling | first8 = T. | title = Frequent germ-line mutations of the MEN1, CASR, and HRPT2/CDC73 genes in young patients with clinically non-familial primary hyperparathyroidism. | journal = Horm Cancer | volume = 3 | issue = 1-2 | pages = 44-51 | month = Apr | year = 2012 | doi = 10.1007/s12672-011-0100-8 | PMID = 22187299 }}</ref><ref name=pmid23652676>{{Cite journal | last1 = Hendy | first1 = GN. | last2 = Cole | first2 = DE. | title = Genetic defects associated with familial and sporadic hyperparathyroidism. | journal = Front Horm Res | volume = 41 | issue = | pages = 149-65 | month = | year = 2013 | doi = 10.1159/000345675 | PMID = 23652676 }}</ref> | |||
*MEN1. | |||
*CASR. | |||
*HRPT2/CDC73. | |||
*CDKN1B. | |||
*RET. | |||
====Hypercalcemia DDx==== | |||
Mnemonic ''GRIMED'':<ref>{{Ref TN2006| Emerg.}}</ref> | |||
*Granulomatous disease ([[tuberculosis]], [[sarcoidosis]]). | |||
*Renal disease. | |||
*Immobility. | |||
*Malignancy (esp. squamous cell carcinoma, [[plasmacytoma]]). | |||
*Endocrine (primary hyperparathyroidism, tertiary hyperparathyroidism, familial hypocalciuric hypercalcemia (FHH)). | |||
*Drugs (thiazides ... others). | |||
Note: | |||
*Hyperparathyroidism and FHH are assoc. with an increased PTH.<ref name=Ref_PBoD8_1129>{{Ref PBoD8|1129}}</ref> | |||
**Other causes are assoc. with a decreased PTH. | |||
====Primary hyperparathyroidism==== | ====Primary hyperparathyroidism==== | ||
| Line 16: | Line 69: | ||
Familial causes of primary hyperparathyroidism: | Familial causes of primary hyperparathyroidism: | ||
*[[MEN 1]]. | *[[MEN 1]]. | ||
*[[MEN | *[[MEN 2A]]. | ||
*Familial hypocalciuric hypercalcemia. | *Familial hypocalciuric hypercalcemia. | ||
**Autosomal dominant. | **Autosomal dominant. | ||
**CASR (calcium sensing receptor) gene defect.<ref name=omim601199>{{OMIM|601199}}</ref> | **CASR (calcium sensing receptor) gene defect.<ref name=omim601199>{{OMIM|601199}}</ref> | ||
== | Classic manifestations ''moans, stones, bones, (abdominal) groans, psychiatric overtones''.<ref>{{Cite journal | last1 = Lienert | first1 = D. | last2 = Rege | first2 = S. | title = Moans, stones, groans, bones and psychiatric overtones: lithium-induced hyperparathyroidism. | journal = Aust N Z J Psychiatry | volume = 42 | issue = 2 | pages = 171-3 | month = Feb | year = 2008 | doi = | PMID = 18350681 }} | ||
</ref><ref>URL: [http://www.usmleforum.com/files/forum/2010/1/505388.php http://www.usmleforum.com/files/forum/2010/1/505388.php]. Accessed on: 4 December 2011.</ref> | |||
* | *Moans = bone pain. | ||
* | *Stones = [[nephrolithiasis]] (kidney stones). | ||
* | *Bones = bone pathology, e.g. osteitis fibrosa cystica.<ref>{{Cite journal | last1 = França | first1 = TC. | last2 = Griz | first2 = L. | last3 = Pinho | first3 = J. | last4 = Diniz | first4 = ET. | last5 = Andrade | first5 = LD. | last6 = Lucena | first6 = CS. | last7 = Beserra | first7 = SR. | last8 = Asano | first8 = NM. | last9 = Duarte | first9 = AP. | title = Bisphosphonates can reduce bone hunger after parathyroidectomy in patients with primary hyperparathyroidism and osteitis fibrosa cystica. | journal = Rev Bras Reumatol | volume = 51 | issue = 2 | pages = 131-7 | month = Apr | year = 2011 | doi = | PMID = 21584419 }}</ref> | ||
* | *Groans = constipation. | ||
* | *Psychiatric overtones = CNS pathology. | ||
**Can include: lethargy, fatigue, depression, memory loss, psychosis, ataxia, delirium, and coma. | |||
==Hypoparathyroidism== | |||
*Rare vis-à-vis hyperparathyroidism. | |||
*Classically iatrogenic, i.e. the surgeon removing 'em.<ref name=Ref_PBoD8_1129>{{Ref PBoD8|1129}}</ref> | |||
Other causes:<ref name=Ref_PBoD8_1130>{{Ref PBoD8|1130}}</ref> | |||
*Autoimmune hypoparathyroidism. | |||
*Autosomal dominat hypoparathyroidism. | |||
*Familial isolated hypoparathyroidism. | |||
*Congenital absence ([[DiGeorge syndrome]]). | |||
*Drugs - [[proton pump inhibitors]].<ref name=pmid24736034>{{Cite journal | last1 = Deroux | first1 = A. | last2 = Khouri | first2 = C. | last3 = Chabre | first3 = O. | last4 = Bouillet | first4 = L. | last5 = Casez | first5 = O. | title = Severe acute neurological symptoms related to proton pump inhibitors induced hypomagnesemia responsible for profound hypoparathyroidism with hypocalcemia. | journal = Clin Res Hepatol Gastroenterol | volume = 38 | issue = 5 | pages = e103-5 | month = Oct | year = 2014 | doi = 10.1016/j.clinre.2014.03.005 | PMID = 24736034 }}</ref><ref name=pmid25138239>{{Cite journal | last1 = Toh | first1 = JW. | last2 = Ong | first2 = E. | last3 = Wilson | first3 = R. | title = Hypomagnesaemia associated with long-term use of proton pump inhibitors. | journal = Gastroenterol Rep (Oxf) | volume = | issue = | pages = | month = Aug | year = 2014 | doi = 10.1093/gastro/gou054 | PMID = 25138239 }}</ref> | |||
=Normal parathyroid glands= | =Normal parathyroid glands= | ||
:The [[cytology]] is dealt with in ''[[normal parathyroid cytology]]''. | |||
===General=== | ===General=== | ||
*Identification of normal can be tricky. | *Identification of normal can be tricky. | ||
| Line 49: | Line 114: | ||
***Chief cells - predominant cell type, small, cytoplasm has variable staining (hyperchromatic-clear-eosinophilic). | ***Chief cells - predominant cell type, small, cytoplasm has variable staining (hyperchromatic-clear-eosinophilic). | ||
***Oxyphil cells (''acid staining'' cells<ref>[http://dictionary.reference.com/search?q=oxyphil%20cell http://dictionary.reference.com/search?q=oxyphil%20cell]</ref>) - abundant cytoplasm. | ***Oxyphil cells (''acid staining'' cells<ref>[http://dictionary.reference.com/search?q=oxyphil%20cell http://dictionary.reference.com/search?q=oxyphil%20cell]</ref>) - abundant cytoplasm. | ||
***Adipocytes - | ***Adipocytes - dependent on age, body habitus, PT hormone, size of gland.<ref name=pmid7551007>{{Cite journal | last1 = Iwasaki | first1 = A. | last2 = Shan | first2 = L. | last3 = Kawano | first3 = I. | last4 = Nakamura | first4 = M. | last5 = Utsuno | first5 = H. | last6 = Kobayashi | first6 = A. | last7 = Kuma | first7 = K. | last8 = Kakudo | first8 = K. | title = Quantitative analysis of stromal fat content of human parathyroid glands associated with thyroid diseases using computer image analysis. | journal = Pathol Int | volume = 45 | issue = 7 | pages = 483-6 | month = Jul | year = 1995 | doi = | PMID = 7551007 }}</ref> | ||
****Increased with age, may be used to help differentiate from thyroid - '''key feature'''. | |||
====Images==== | |||
<gallery> | |||
Image:Parathyroid_gland_intermed_mag.jpg | Parathyroid gland - intermed. mag. (WC) | |||
Image:Parathyroid_gland_high_mag.jpg | Parathyroid gland - cropped - high mag. (WC) | |||
Image:Parathyroid_gland_high_mag_cropped.jpg | Parathyroid gland - high mag. (WC) | |||
</gallery> | |||
www: | |||
*[http://library.med.utah.edu/WebPath/ENDOHTML/ENDO031.html Parathyroid - med.utah.edu]. | |||
*[http://pathology.mc.duke.edu/research/PTH225.html Histology - several images. - pathology.mc.duke.edu]. | |||
====Parathyroid cell types==== | |||
{| class="wikitable" | {| class="wikitable" | ||
! Name | |||
! Staining (cytoplasm) | |||
! Quantity of cells | |||
! Cytoplasm (quantity) | |||
! Function | |||
! Image | |||
|- | |||
| (parathyroid) chief cells | |||
| intense hyperchromatic to eosinophilic (see note) | |||
| abundant | |||
| moderate | |||
| manufacture parathyroid <br>hormone (PTH) | |||
| [[Image:Parathyroid adenoma - chief cells -- high mag.jpg|thumb|center|85px|Chief cells (WC)]] | |||
|- | |||
| oxyphil cells | |||
| moderate/light hyperchromatic to eosinophilic | |||
| rare | |||
| abundant | |||
| ? | |||
| [[Image:Parathyroid adenoma - oxyphil cells -- high mag.jpg|thumb|center|85px|Oxyphil cells (WC)]] | |||
|} | |} | ||
Notes: | Notes: | ||
*Cytoplasmic staining varies considerably on H&E preparations - it may vary from hyperchromatic<ref>[http://www.deltagen.com/target/histologyatlas/atlas_files/endocrine/parathyroid_and_thyroid_glands_20x.jpg http://www.deltagen.com/target/histologyatlas/atlas_files/endocrine/parathyroid_and_thyroid_glands_20x.jpg]</ref> to clear to eosinophilic<ref>[http://instruction.cvhs.okstate.edu/Histology/HistologyReference/hrendo.htm http://instruction.cvhs.okstate.edu/Histology/HistologyReference/hrendo.htm]</ref> | *Cytoplasmic staining varies considerably on H&E preparations - it may vary from hyperchromatic<ref>[http://www.deltagen.com/target/histologyatlas/atlas_files/endocrine/parathyroid_and_thyroid_glands_20x.jpg http://www.deltagen.com/target/histologyatlas/atlas_files/endocrine/parathyroid_and_thyroid_glands_20x.jpg]</ref> to clear to eosinophilic.<ref>[http://instruction.cvhs.okstate.edu/Histology/HistologyReference/hrendo.htm http://instruction.cvhs.okstate.edu/Histology/HistologyReference/hrendo.htm]</ref> | ||
*Chief cells tend to stain more intensely than oxyphil cells. | *Chief cells tend to stain more intensely than oxyphil cells. | ||
Thyroid | ====Thyroid versus parathyroid==== | ||
*Parathyroid cytoplasm: | *Parathyroid cytoplasm: | ||
**Hyperchromatic. | **Hyperchromatic. | ||
Notes: | |||
*Thyroid often has birefringent (calcium oxalate) crystals (60 of 80 cases) whereas parathyroid less often does (2 or 20 cases).<ref name=pmid24618617>{{cite journal |authors=Wong KS, Lewis JS, Gottipati S, Chernock RD |title=Utility of birefringent crystal identification by polarized light microscopy in distinguishing thyroid from parathyroid tissue on intraoperative frozen sections |journal=Am J Surg Pathol |volume=38 |issue=9 |pages=1212–9 |date=September 2014 |pmid=24618617 |doi=10.1097/PAS.0000000000000204 |url=}}</ref> | |||
*Thyroid usually follicular - though parathyroid occasionally is pseudofollicular. | |||
====Parathyroid versus lymphoid tissue==== | |||
*Parathyroid: | *Parathyroid: | ||
**No germinal centres. | **No germinal centres. | ||
**Gland-like/follicular-like arrangement | **Gland-like/follicular-like arrangement may be present but usually much smaller than normal thyroid follicles. | ||
***May be confused with thyroid microfollicules. | |||
**Occasional cell with rim of clear cytoplasm (oxyphil?). | **Occasional cell with rim of clear cytoplasm (oxyphil?). | ||
**Nuclei are different: | |||
***Slightly larger than in lymphocytes (1.2-1.5x the size) | |||
***Stippled chromatin (unlike lymphocytes). | |||
Images: | Images: | ||
*[http:// | *[http://www.deltagen.com/target/histologyatlas/atlas_files/endocrine/parathyroid_and_thyroid_glands_20x.jpg Parathyroid image (deltagen.com)]. | ||
*[http:// | *[http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1770637/figure/f1/ Parathyroid gland (nih.gov)].<ref name=pmid15790694>{{Cite journal | last1 = Johnson | first1 = SJ. | last2 = Sheffield | first2 = EA. | last3 = McNicol | first3 = AM. | title = Best practice no 183. Examination of parathyroid gland specimens. | journal = J Clin Pathol | volume = 58 | issue = 4 | pages = 338-42 | month = Apr | year = 2005 | doi = 10.1136/jcp.2002.002550 | PMID = 15790694 | pmc = 1770637 }}</ref> | ||
===IHC=== | |||
*GATA3 +ve (>98%<ref name=pmid27097544>{{Cite journal | last1 = Takada | first1 = N. | last2 = Hirokawa | first2 = M. | last3 = Suzuki | first3 = A. | last4 = Higuchi | first4 = M. | last5 = Kuma | first5 = S. | last6 = Miyauchi | first6 = A. | title = Diagnostic value of GATA-3 in cytological identification of parathyroid tissues. | journal = Endocr J | volume = 63 | issue = 7 | pages = 621-6 | month = Jul | year = 2016 | doi = 10.1507/endocrj.EJ15-0700 | PMID = 27097544 }}</ref>). | |||
*PTH -ve/+ve (~33%<ref name=pmid27097544/>). | |||
*Chromogranin A +ve (~80%<ref name=pmid27097544/>). | |||
*AE1/AE3 +ve.{{fact}}<!-- {{Cite journal | last1 = Piciu | first1 = D. | last2 = Irimie | first2 = A. | last3 = Kontogeorgos | first3 = G. | last4 = Piciu | first4 = A. | last5 = Buiga | first5 = R. | title = Highly aggressive pathology of non-functional parathyroid carcinoma. | journal = Orphanet J Rare Dis | volume = 8 | issue = | pages = 115 | month = Aug | year = 2013 | doi = 10.1186/1750-1172-8-115 | PMID = 23915575 }} --> | |||
=Specific entities= | =Specific entities= | ||
==Parathyroid hyperplasia== | ==Parathyroid hyperplasia== | ||
{{Main|Parathyroid hyperplasia}} | |||
==Parathyroid adenoma== | ==Parathyroid adenoma== | ||
{{Main|Parathyroid adenoma}} | |||
==Parathyroid carcinoma== | ==Parathyroid carcinoma== | ||
{{Main|Parathyroid carcinoma}} | |||
=See also= | =See also= | ||
Latest revision as of 17:24, 22 February 2021
The parathyroid glands are an endocrine organ that is important in calcium regulation. They often make an appearance in the context of thyroid surgery.
They produce parathyroid hormone (PTH). PTH acts to increase serum calcium and is important in the regulation of the calcium balance.
Clinical
Hyperparathyroidism
- Definition: increased secretion of parathyroid hormone (PTH).[1]
What PTH does:[1]
- Increase serum calcium.
- Decrease serum phosphate.
Classification
- Primary.
- Secondary.
- Tertiary.
Overview in a table
| Type | PTH | Calcium | Common causes |
|---|---|---|---|
| Primary hyperparathyroidism | high | high | parathyroid adenoma (~85-90% of cases), parathyroid hyperplasia (~10-15% of cases) |
| Secondary hyperparathyroidism | high | low or normal | chronic renal failure, vitamin D deficiency[2] |
| Tertiary hyperparathyroidism | high | high | persistent hyperparathyroidism after renal transplant;[3] arises in the context of secondary hyperparathyroidism[4] |
Genetics
Genes implicated in hyperparathyroidism:[5][6]
- MEN1.
- CASR.
- HRPT2/CDC73.
- CDKN1B.
- RET.
Hypercalcemia DDx
Mnemonic GRIMED:[7]
- Granulomatous disease (tuberculosis, sarcoidosis).
- Renal disease.
- Immobility.
- Malignancy (esp. squamous cell carcinoma, plasmacytoma).
- Endocrine (primary hyperparathyroidism, tertiary hyperparathyroidism, familial hypocalciuric hypercalcemia (FHH)).
- Drugs (thiazides ... others).
Note:
- Hyperparathyroidism and FHH are assoc. with an increased PTH.[8]
- Other causes are assoc. with a decreased PTH.
Primary hyperparathyroidism
Cause:[9]
- Parathyroid adenoma ~90%.
- Parathyroid hyperplasia ~10%.
- Parathyroid carcinoma ~1%.
Familial causes of primary hyperparathyroidism:
- MEN 1.
- MEN 2A.
- Familial hypocalciuric hypercalcemia.
- Autosomal dominant.
- CASR (calcium sensing receptor) gene defect.[10]
Classic manifestations moans, stones, bones, (abdominal) groans, psychiatric overtones.[11][12]
- Moans = bone pain.
- Stones = nephrolithiasis (kidney stones).
- Bones = bone pathology, e.g. osteitis fibrosa cystica.[13]
- Groans = constipation.
- Psychiatric overtones = CNS pathology.
- Can include: lethargy, fatigue, depression, memory loss, psychosis, ataxia, delirium, and coma.
Hypoparathyroidism
- Rare vis-à-vis hyperparathyroidism.
- Classically iatrogenic, i.e. the surgeon removing 'em.[8]
Other causes:[14]
- Autoimmune hypoparathyroidism.
- Autosomal dominat hypoparathyroidism.
- Familial isolated hypoparathyroidism.
- Congenital absence (DiGeorge syndrome).
- Drugs - proton pump inhibitors.[15][16]
Normal parathyroid glands
- The cytology is dealt with in normal parathyroid cytology.
General
- Identification of normal can be tricky.
Gross
- No distinctive features - surgeons thus send 'em to pathologists.
Microscopic
Features:[17]
- Low power:
- May vaguely resemble lymphoid tissue - may have hyperchromatic cytoplasm.
- Does not have follicular centres like a lymph node.
- May form gland-like structure and vaguely resemble the thyroid at low power.
- Cytoplasm may be clear[18] - key feature.
- Surrounded by a thin fibrous capsule.
- May vaguely resemble lymphoid tissue - may have hyperchromatic cytoplasm.
- High power:
- Mixed cell population:[19]
- Chief cells - predominant cell type, small, cytoplasm has variable staining (hyperchromatic-clear-eosinophilic).
- Oxyphil cells (acid staining cells[20]) - abundant cytoplasm.
- Adipocytes - dependent on age, body habitus, PT hormone, size of gland.[21]
- Increased with age, may be used to help differentiate from thyroid - key feature.
- Mixed cell population:[19]
Images
www:
Parathyroid cell types
| Name | Staining (cytoplasm) | Quantity of cells | Cytoplasm (quantity) | Function | Image |
|---|---|---|---|---|---|
| (parathyroid) chief cells | intense hyperchromatic to eosinophilic (see note) | abundant | moderate | manufacture parathyroid hormone (PTH) |
|
| oxyphil cells | moderate/light hyperchromatic to eosinophilic | rare | abundant | ? |
Notes:
- Cytoplasmic staining varies considerably on H&E preparations - it may vary from hyperchromatic[22] to clear to eosinophilic.[23]
- Chief cells tend to stain more intensely than oxyphil cells.
Thyroid versus parathyroid
- Parathyroid cytoplasm:
- Hyperchromatic.
Notes:
- Thyroid often has birefringent (calcium oxalate) crystals (60 of 80 cases) whereas parathyroid less often does (2 or 20 cases).[24]
- Thyroid usually follicular - though parathyroid occasionally is pseudofollicular.
Parathyroid versus lymphoid tissue
- Parathyroid:
- No germinal centres.
- Gland-like/follicular-like arrangement may be present but usually much smaller than normal thyroid follicles.
- May be confused with thyroid microfollicules.
- Occasional cell with rim of clear cytoplasm (oxyphil?).
- Nuclei are different:
- Slightly larger than in lymphocytes (1.2-1.5x the size)
- Stippled chromatin (unlike lymphocytes).
Images:
IHC
- GATA3 +ve (>98%[26]).
- PTH -ve/+ve (~33%[26]).
- Chromogranin A +ve (~80%[26]).
- AE1/AE3 +ve.[citation needed]
Specific entities
Parathyroid hyperplasia
Main article: Parathyroid hyperplasia
Parathyroid adenoma
Main article: Parathyroid adenoma
Parathyroid carcinoma
Main article: Parathyroid carcinoma
See also
References
- ↑ 1.0 1.1 URL: http://emedicine.medscape.com/article/127351-overview. Accessed on: 24 January 2013.
- ↑ URL: http://emedicine.medscape.com/article/127351-overview#aw2aab6b5. Accessed on: 24 January 2013.
- ↑ URL: http://emedicine.medscape.com/article/127351-overview#aw2aab6b6. Accessed on: 24 January 2013.
- ↑ Duan, K.; Gomez Hernandez, K.; Mete, O. (Oct 2015). "Clinicopathological correlates of hyperparathyroidism.". J Clin Pathol 68 (10): 771-87. doi:10.1136/jclinpath-2015-203186. PMID 26163537.
- ↑ Starker, LF.; Akerström, T.; Long, WD.; Delgado-Verdugo, A.; Donovan, P.; Udelsman, R.; Lifton, RP.; Carling, T. (Apr 2012). "Frequent germ-line mutations of the MEN1, CASR, and HRPT2/CDC73 genes in young patients with clinically non-familial primary hyperparathyroidism.". Horm Cancer 3 (1-2): 44-51. doi:10.1007/s12672-011-0100-8. PMID 22187299.
- ↑ Hendy, GN.; Cole, DE. (2013). "Genetic defects associated with familial and sporadic hyperparathyroidism.". Front Horm Res 41: 149-65. doi:10.1159/000345675. PMID 23652676.
- ↑ Shiau, Carolyn; Toren, Andrew (2006). Toronto Notes 2006: Comprehensive Medical Reference (Review for MCCQE 1 and USMLE Step 2) (22nd edition (2006) ed.). Toronto Notes for Medical Students, Inc.. pp. Emerg.. ISBN 978-0968592861.
- ↑ 8.0 8.1 Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; Aster, Jon (2009). Robbins and Cotran pathologic basis of disease (8th ed.). Elsevier Saunders. pp. 1129. ISBN 978-1416031215.
- ↑ Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; Aster, Jon (2009). Robbins and Cotran pathologic basis of disease (8th ed.). Elsevier Saunders. pp. 1127. ISBN 978-1416031215.
- ↑ Online 'Mendelian Inheritance in Man' (OMIM) 601199
- ↑ Lienert, D.; Rege, S. (Feb 2008). "Moans, stones, groans, bones and psychiatric overtones: lithium-induced hyperparathyroidism.". Aust N Z J Psychiatry 42 (2): 171-3. PMID 18350681.
- ↑ URL: http://www.usmleforum.com/files/forum/2010/1/505388.php. Accessed on: 4 December 2011.
- ↑ França, TC.; Griz, L.; Pinho, J.; Diniz, ET.; Andrade, LD.; Lucena, CS.; Beserra, SR.; Asano, NM. et al. (Apr 2011). "Bisphosphonates can reduce bone hunger after parathyroidectomy in patients with primary hyperparathyroidism and osteitis fibrosa cystica.". Rev Bras Reumatol 51 (2): 131-7. PMID 21584419.
- ↑ Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; Aster, Jon (2009). Robbins and Cotran pathologic basis of disease (8th ed.). Elsevier Saunders. pp. 1130. ISBN 978-1416031215.
- ↑ Deroux, A.; Khouri, C.; Chabre, O.; Bouillet, L.; Casez, O. (Oct 2014). "Severe acute neurological symptoms related to proton pump inhibitors induced hypomagnesemia responsible for profound hypoparathyroidism with hypocalcemia.". Clin Res Hepatol Gastroenterol 38 (5): e103-5. doi:10.1016/j.clinre.2014.03.005. PMID 24736034.
- ↑ Toh, JW.; Ong, E.; Wilson, R. (Aug 2014). "Hypomagnesaemia associated with long-term use of proton pump inhibitors.". Gastroenterol Rep (Oxf). doi:10.1093/gastro/gou054. PMID 25138239.
- ↑ http://www.medicalhistology.us/twiki/pub/Main/ChapterFourteenSlides/b56b_parathyroid_40x_he_labeled.jpg
- ↑ http://pathology.mc.duke.edu/research/Histo_course/parathyroid2.jpg
- ↑ http://www.bu.edu/histology/p/15002loa.htm
- ↑ http://dictionary.reference.com/search?q=oxyphil%20cell
- ↑ Iwasaki, A.; Shan, L.; Kawano, I.; Nakamura, M.; Utsuno, H.; Kobayashi, A.; Kuma, K.; Kakudo, K. (Jul 1995). "Quantitative analysis of stromal fat content of human parathyroid glands associated with thyroid diseases using computer image analysis.". Pathol Int 45 (7): 483-6. PMID 7551007.
- ↑ http://www.deltagen.com/target/histologyatlas/atlas_files/endocrine/parathyroid_and_thyroid_glands_20x.jpg
- ↑ http://instruction.cvhs.okstate.edu/Histology/HistologyReference/hrendo.htm
- ↑ Wong KS, Lewis JS, Gottipati S, Chernock RD (September 2014). "Utility of birefringent crystal identification by polarized light microscopy in distinguishing thyroid from parathyroid tissue on intraoperative frozen sections". Am J Surg Pathol 38 (9): 1212–9. doi:10.1097/PAS.0000000000000204. PMID 24618617.
- ↑ Johnson, SJ.; Sheffield, EA.; McNicol, AM. (Apr 2005). "Best practice no 183. Examination of parathyroid gland specimens.". J Clin Pathol 58 (4): 338-42. doi:10.1136/jcp.2002.002550. PMC 1770637. PMID 15790694. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1770637/.
- ↑ 26.0 26.1 26.2 Takada, N.; Hirokawa, M.; Suzuki, A.; Higuchi, M.; Kuma, S.; Miyauchi, A. (Jul 2016). "Diagnostic value of GATA-3 in cytological identification of parathyroid tissues.". Endocr J 63 (7): 621-6. doi:10.1507/endocrj.EJ15-0700. PMID 27097544.